Surgical Treatment
Surgical treatment is usually an additional or alternative treatment option for women with pain not responding to medical treatment, women trying to conceive, but have been unsuccessful, or women with recurrence of symptoms. Surgery can help identify or rule out endometriosis.
When choosing the best treatment approach one needs to take into account various factors such as potential risks and benefits, patient reference, previous history etc. Surgery is still widely considered the diagnostic gold standard, however it is not without risks (see below) which is why many women usually receive medical treatment as the first approach (see Medical Treatment). This can be seen as 'empirical treatment' which means that it is also used a diagnostic test. If the symptoms get better, then there is a reasonable chance that it is endometriosis and if the side effects are acceptable to the woman and she is not trying to conceive in the close future, medical treatment is continued.
Surgery is an options If:
- women are trying to conceive in the close future and have been unsuccessful or are in pain
- side effects of the medications are unacceptable
- medication does not significantly improve the symptoms
- women would prefer surgery and understand the risks and possible outcomes.
LAPAROSCOPY
Laparoscopy (“keyhole surgery”) is done under general anaesthesia. It is a technique in which a thin telescope is inserted into the abdomen to inspect the pelvic organs. An approximately 5-10mm cut is made within or under the belly button or, less often, below your left rib cage and your stomach is filled with gas (CO2) which will be released at the end of the procedure. This distension of the stomach allows the surgeon to inspect the pelvic organs to investigate possible reasons for your symptoms such as endometriosis. Another small, approximately 5mm incision is made close to the pubic hairline or on the side. This incision will allow the surgeon to insert a long instrument into the abdomen and push the bowel out of the way to get a better view.
A further one or two (rarely three) incisions may be made to allow insertion of instruments for further investigation and possibly treatment of affect areas. For example, the surgeon may remove the affected areas, divide adhesions or drain and remove cysts.
You may be required to have drugs prior to or after surgery. If the tissue is particularly vascular or organs are stuck together (abdominal adhesions) your surgery may entail partial surgical treatment followed by drugs and a second planned procedure in the interval (see below). In other words, in rare cases surgery will be undertaken in two stages to optimise complete removal of disease.
 Surgery is mostly done laparoscopically. This procedure is also known as keyhole surgery or minimally invasive surgery.
Surgery is mostly done laparoscopically. This procedure is also known as keyhole surgery or minimally invasive surgery.
Minor Surgery
Minor surgery will involve inspection and burning or removal of the endometriosis tissue or spots.
- Usually you would be admitted and discharged on the day of surgery. However, the duration of your stay depends on the extent of endometriosis/treatment.
- Only rarely, you may have a catheter (tube in the bladder) overnight.
- Adhesions (scar tissue) would be divided or removed.
- An endometrioma or chocolate cyst (cyst filled with endometriotic fluid) will be opened, drained and ideally removed. Care will be taken to preserve as much normal ovarian tissue as possible and reconstruct the ovary where required.
- You may also have a PCA (patient controlled analgesia) overnight where you have the control of pain relief medication which you may administer yourself by pressing a button.
- You may be asked to see your doctor/nurse to remove the stitches after one week. However, most suture material nowadays dissolves on its own. Please confirm this with you doctor or nurse.
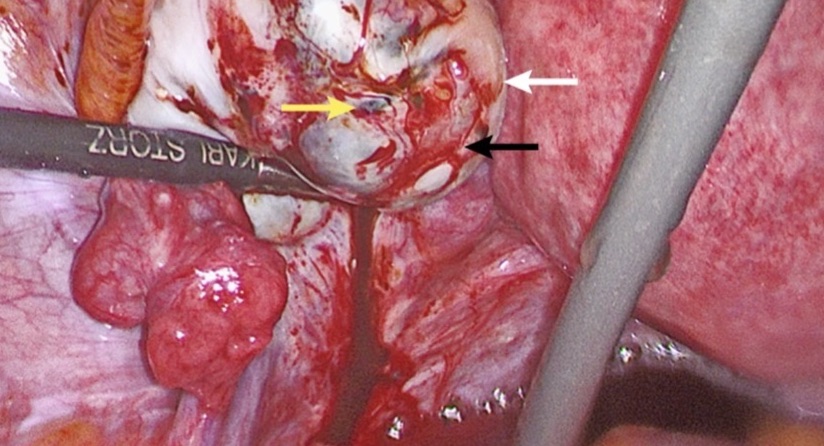 Left ovary with draining endometriotic (chocolate) cyst (white arrow; panel c). Superficial red lesions (black arrow) and black lesions (yellow arrow) are also present.
Left ovary with draining endometriotic (chocolate) cyst (white arrow; panel c). Superficial red lesions (black arrow) and black lesions (yellow arrow) are also present.
MAJOR SURGERY
Extensive surgery is also usually achieved through the telescope, though a slightly longer duration of stay may be needed.
This could involve:
- Cutting away the endometriosis-affected tissue
- Releasing ovaries
- Releasing adhesions and removing the tissue affected by endometriosis around the back and the side of the uterus (womb), around the bladder and ureter (tubes that carry urine from kidneys to the bladder) and the space between the rectum (end portion of large bowel) and the vagina
- Dissecting the ureters to be able to remove endometriosis tissue
- Operating and possibly removing parts of bowel
Surgical Risks
The risk of a major complication of laparoscopic surgery in general is 1 in 1,000 (uncommon). However, the more extensive the disease the higher the risks. Specific risks listed below will be discussed in detail by the members of the surgical team when you sign the consent form for the operation.
If any of these complications occur, a laparatomy (open surgery through a larger cut) may need to be undertaken to correct the damage or to stop bleeding. This risk is rare.
Women who are obese or very thin; who have significant pathology; who have had previous surgery; or who have pre-existing medical conditions must understand that the quoted risks for serious or frequent complications will be increased. The risk of serious complications at laparoscopy also increases if an additional therapeutic procedure is performed.
The above descriptors are based on the Royal College of Obstetricians and Gynaecologists Clinical Governance Advice No. 7 Presenting Information on Risk.
| Term |
Equivalent numerical ratio |
Colloquial equivalent |
|
Very common |
1/1 to 1/10 |
A person in a family |
|
Common |
1/10 to 1/100 |
A person in a street |
|
Uncommon |
1/100 to 1/1,000 |
A person in a village |
|
Rare |
1/1,000 to 1/10,000 |
A person in a small town |
|
Very rare |
Less than 1/10,000 |
A person in a large town |
FREQUENT RISKS
Frequent risks are usually mild and self-limiting.They may include:
- bruising
- shoulder-tip pain
- wound gaping
- infection
- scarring
As with all surgery the associated risks may include:
- Infection, bleeding and scarring/adhesion formation.
- Damage to internal organs such as bladder, ureters, blood vessels, nerves and bowel. This risk has been described as up to 1:100 (common).
- Extensive surgery in the pelvis may result in delay in return of bladder function. Occasionally you may need to self-catheterise in the short term and very rarely in the long-term.
- If the ureters are involved, then a stent (tube) may be passed via a telescope before and during endometriosis surgery. The stent will be removed as a day case usually 6 weeks later.
- If the ureter is cut it is possible that a cut will be required in the abdomen to re-join it.
- Bowel damage can result in infection and an abscess. This may require draining with a small tube; occasionally it will require further laparoscopic or open surgery to correct the problem.
- Delayed complications include bowel leakage, haematoma (collection of blood in the abdomen) or a fistula (passageway between two hollow organs or the outside) that can occur after the procedure. In addition, if a piece of bowel has had to be removed then there may be changes to the way the bowels work in the future. These changes usually resolve over a period of weeks to months.
- Loss of a tube or ovary due to bleeding.
SERIOUS RISKS
- Serious risks include damage to the bowel, bladder, ureters, uterus or major blood vessels which would require immediate repair by laparoscopy or laparotomy (open surgery is uncommon). However, up to 15% of bowel injuries might not be diagnosed at the time of laparoscopy.
- Failure to gain entry to the abdominal cavity and to complete the intended procedure.
- Hernia at site of entry (less than 1 in 100; common).
- Thromboembolic complications (rare or very rare).
- 3 in 100,000 women (very rare) undergoing laparoscopy may die as a result of complications.
- Blood transfusions are rarely necessary

